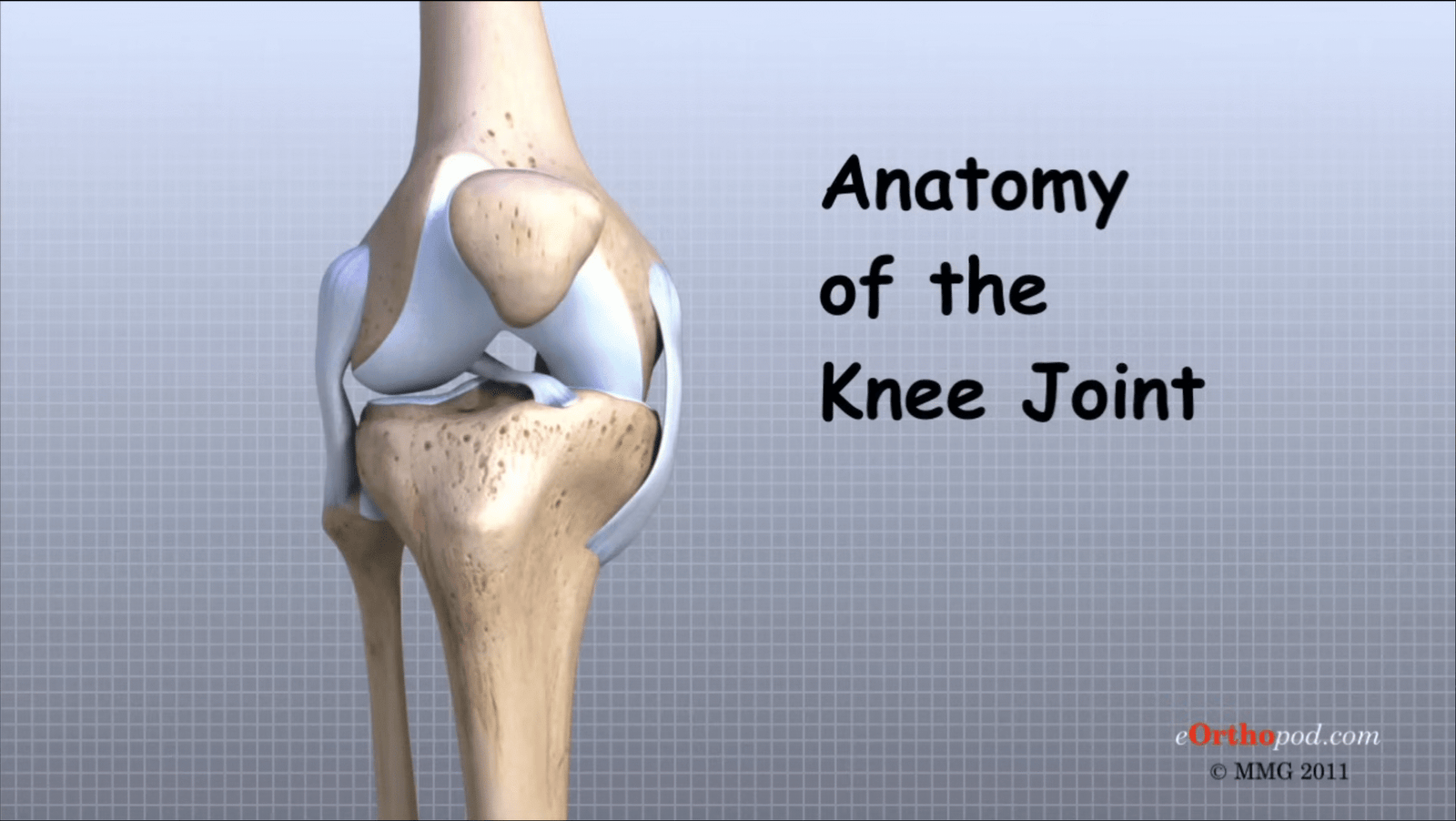
This section helps you understand your ACL injury, surgery, and recovery in a simple way.
Recovery after ACL surgery is not only about exercises. It is also about knowing:
what happened to your knee
what to expect after surgery
how recovery usually progresses
what is normal
when to be careful
how to return safely to activity
Our goal is to help you feel informed, confident, and supported throughout your recovery.
The ACL (anterior cruciate ligament) is one of the main ligaments inside your knee. It helps keep your knee stable, especially during:
When the ACL is injured, your knee may feel:
Sometimes, other parts of the knee may also be affected, such as:
Why this matters:
Understanding the injured structures helps you better understand why rehabilitation takes time and why your recovery plan must be done carefully.
Many ACL injuries happen without direct contact. This is called a non-contact injury.
This can happen during:
Some ACL injuries also happen from direct contact, such as a hit to the knee during sport or a fall.
Why this matters:
Knowing how the injury happened can help you understand your condition and improve awareness for future prevention.


In most cases, a torn ACL is treated with ACL reconstruction (ACLR), not ACL repair.
During ACL reconstruction, a graft is used to create a new ligament.
Common graft options
Each graft option has its own advantages and considerations. Your surgeon will choose the most suitable option based on your condition, activity level, and clinical needs.
Important:
The correct term is usually ACL reconstruction, because this is the standard approach in most cases.
Not all ACL reconstructions are done in isolation.
Some patients may also have:
This means your post-operative instructions may be different.
For example, you may have different:
Please follow the individual advice given by your surgeon and physiotherapist.
This website is a general guide and does not replace personalised medical advice.
After ACL reconstruction, it is common to experience:
These early symptoms are often part of the normal healing process.
Recovery is not always a straight line. Some days feel better, and some days may feel harder. At times, progress may slow down or temporarily go backwards.
This does not always mean something is wrong.
However, worsening symptoms should be reviewed by your healthcare team.
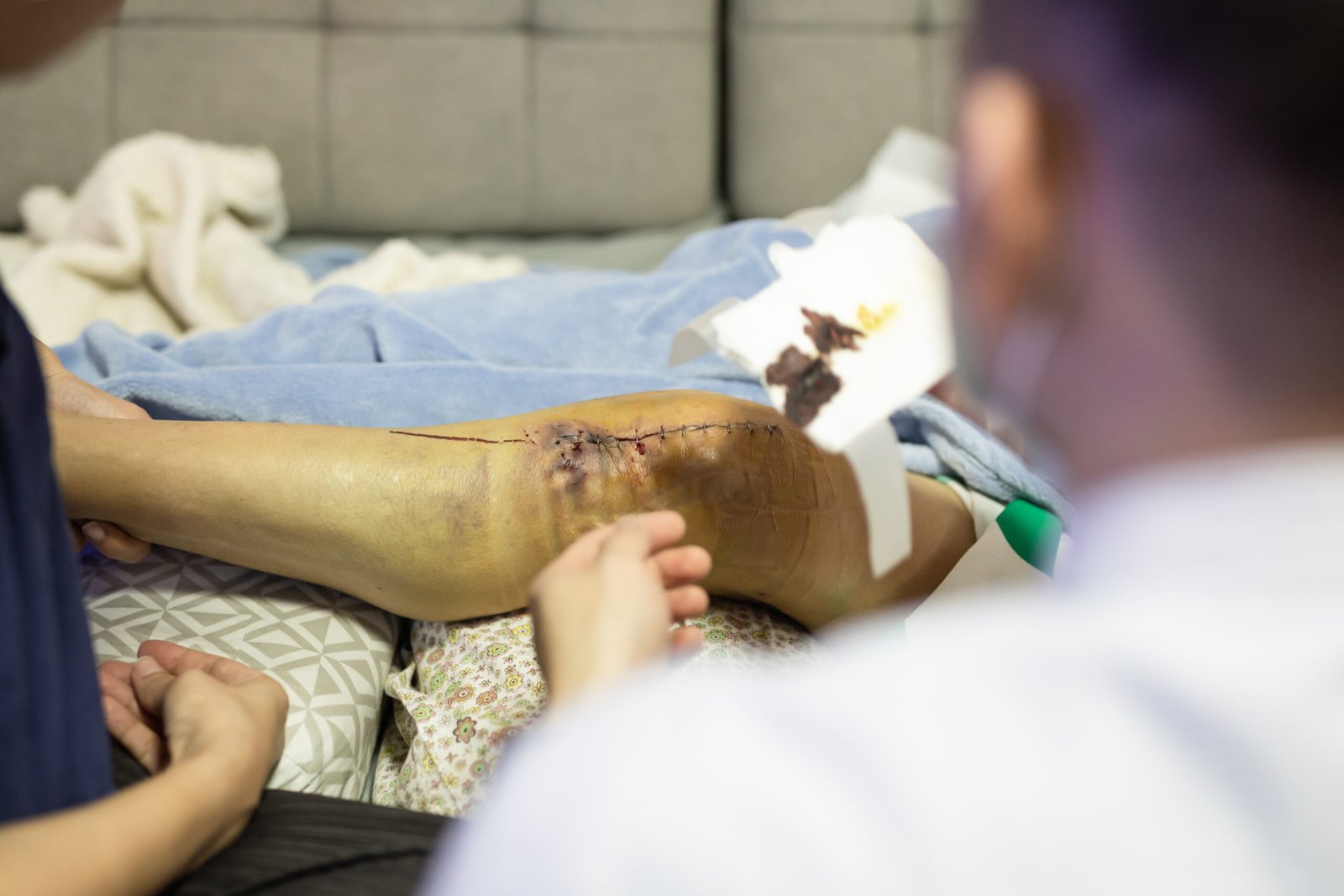
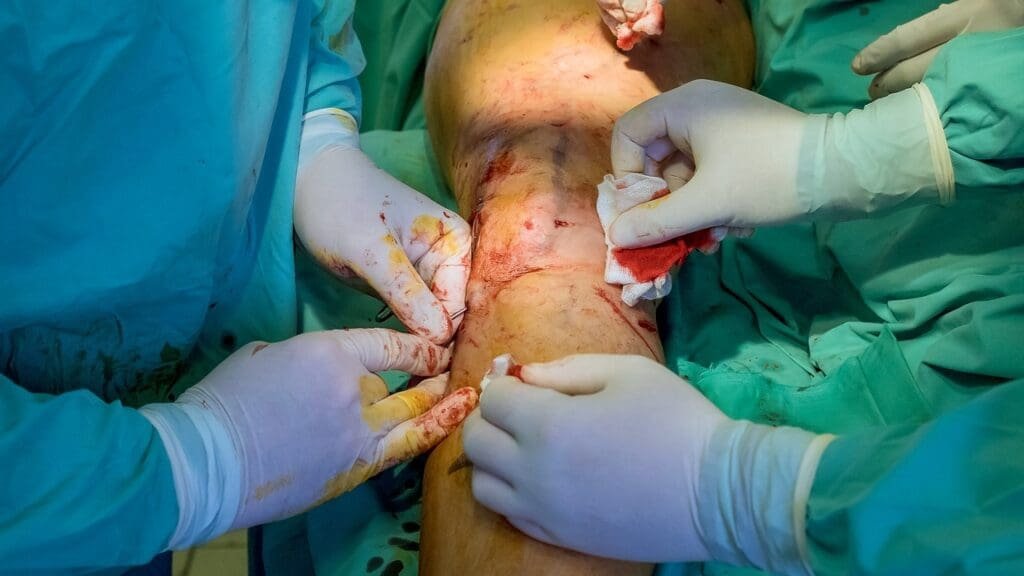
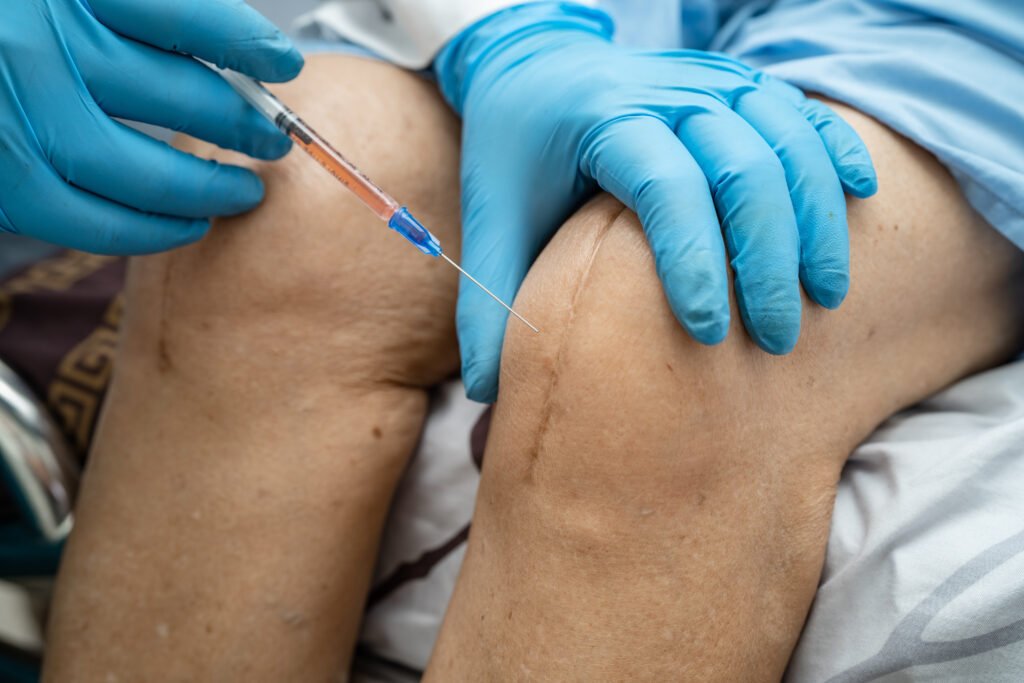
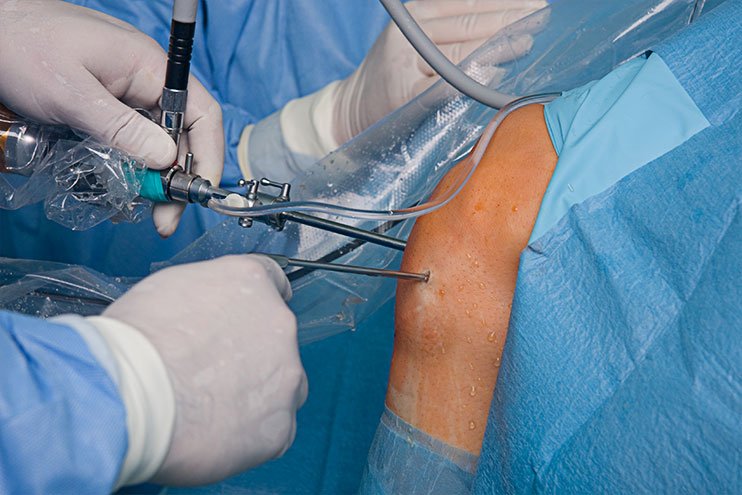
Some complications can happen after ACL reconstruction. These may include:
Some complications can be treated early when identified promptly.
For example:
Early reporting helps prevent delays in recovery.
Prehabilitation means preparing your body before surgery.
This may include improving:
Pre-operative strengthening and preparation can support better recovery after surgery.
Why it helps:
Stronger muscles and better movement before surgery may make early rehabilitation easier and improve recovery outcomes.
How rehabilitation progresses
In SPEAR, rehabilitation is guided by criteria-based progression, not by time alone.
This means you move forward when your knee is showing the right signs of recovery, such as:
Your recovery timeline may not be exactly the same as someone else’s.
Progress depends on:
The calendar is a guide. Your readiness is more important.
.
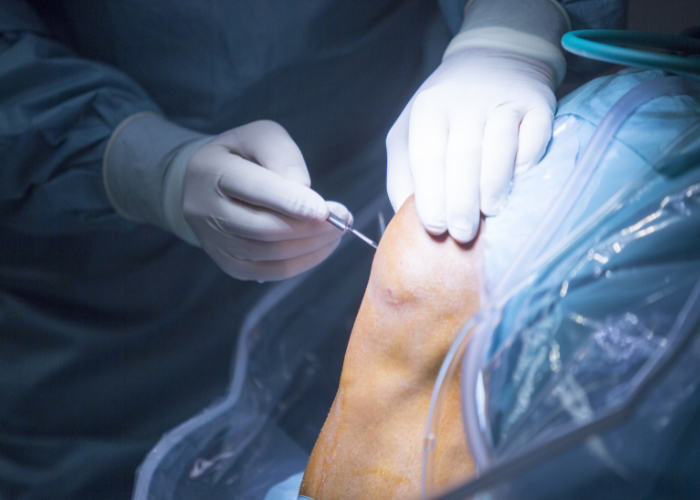
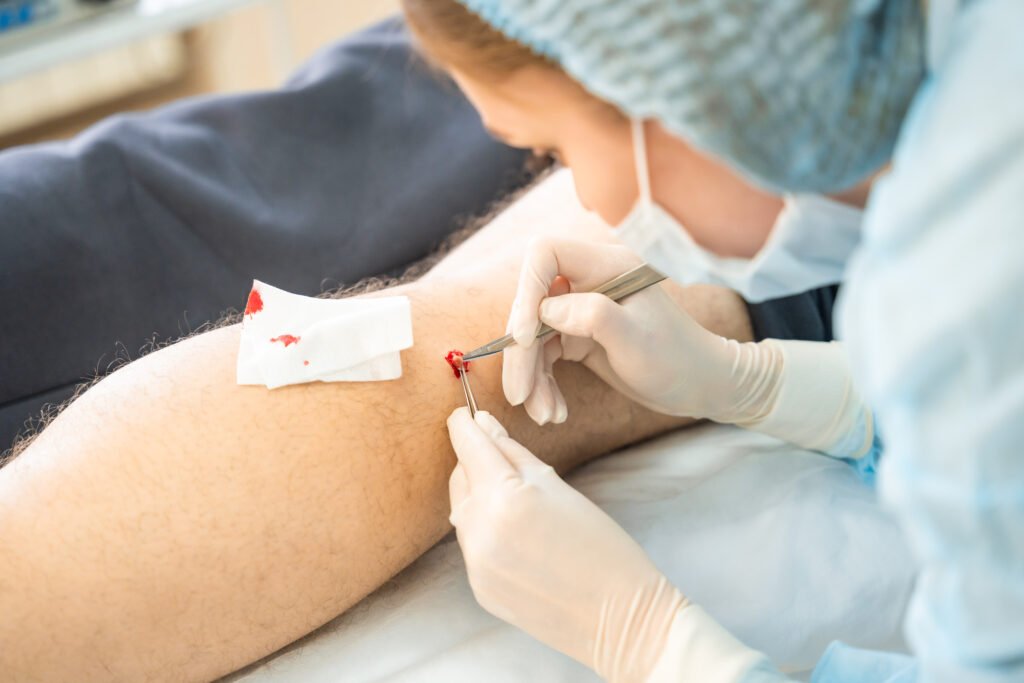
Recovery is not only about doing exercises. Good recovery also depends on:
Knowing when to:
The quadriceps and hamstrings are important because they help support and control the knee.
This means how well your body controls movement, balance, and alignment during activity.
Good movement quality is important for safe progression and reducing re-injury risk.
Good recovery is built on safe progression, not rushing.
Returning to normal activity is not the same as returning to sport.
These stages are different:
Safe return should consider:
Return to sport should not be based on time alone.
You should be physically and mentally ready before progressing.
Even after ACL reconstruction, there is still a risk of:
This risk may increase if:
Safe rehabilitation, good strength, movement control, and readiness-based progression can help reduce this risk.
Please be careful and do not push through warning signs.
Do not progress just because a certain number of weeks has passed.
Progress only when your symptoms and movement are improving safely.

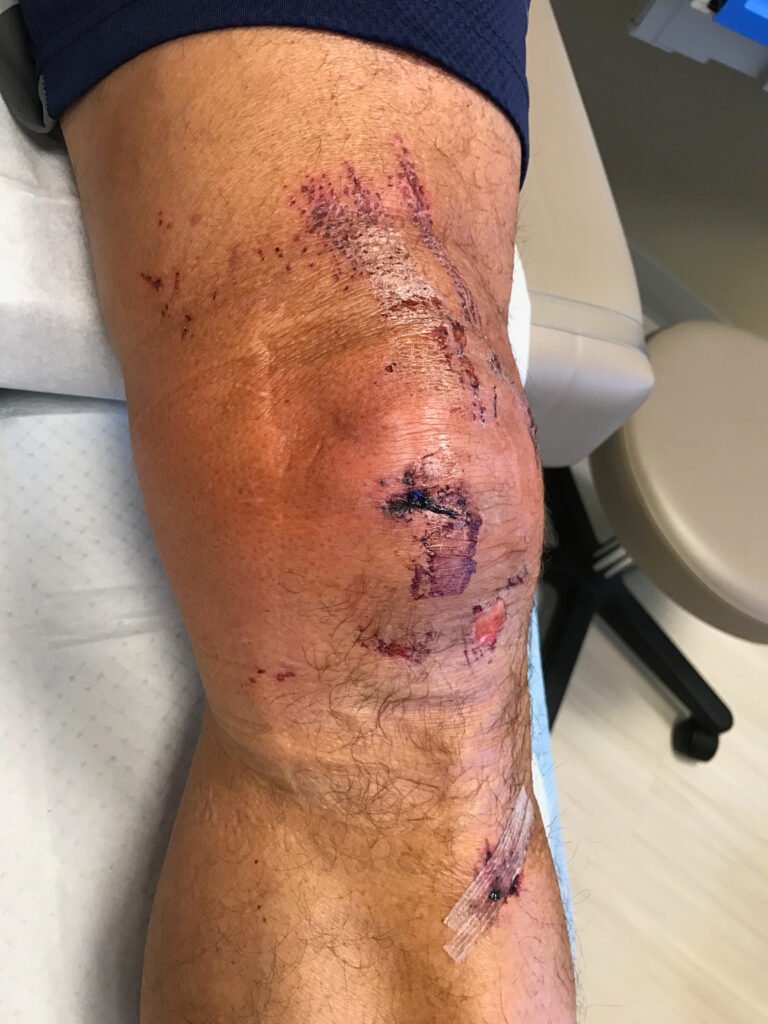
Recovery is a team process.
You may be supported by:
Support is important because recovery can be physical, emotional, and mental.
You do not have to go through recovery alone.
Frequently Asked Questions (FAQ)
Every person heals at a different rate. Your progress depends on your symptoms, healing, strength, confidence, and the type of surgery you had.
Yes. It is common to feel worried, uncertain, or less confident after ACL surgery. This is part of recovery for many people.
Recovery is not always linear. Some days may feel slower or harder. This can happen even when healing is progressing.
No. Time alone is not enough. Your knee should be assessed based on readiness, strength, movement quality, and confidence.
Your rehabilitation restrictions may be different. Always follow the individual advice from your surgeon and physiotherapist.
For more trusted information, please refer to:
This section can be updated with trusted links and resources for patients who want to read more.